Why Do You Suction a Baby's Mouth First
Labour and Delivery Care Module: 7. Neonatal Resuscitation
Written report Session 7 Neonatal Resuscitation
Introduction
The moment when a baby is born is also the fourth dimension when the birth attendant has to make a very rapid assessment of the status of the newborn to decide whether it needs helping to breathe. Within a few seconds you have to be able to identify the general danger signs in a newborn that tell you to intervene chop-chop to protect information technology from developing serious complications, or even dying, considering it is not able to go enough oxygen into its torso. Of class, most babies breathe spontaneously every bit soon as they are born and all yous need to practice is follow the steps of bones newborn care, which were briefly outlined in Study Session five of this Module. You will learn them in much greater detail in the Module on Postnatal Intendance and the steps volition exist covered once more in the Module on Integrated Management of Newborn and Childhood Illness.
However, in this study session our focus is on newborns who are not breathing well, and what yous need to do in guild to resuscitate them and get them animate normally. Yous will learn how to distinguish between a salubrious babe and i that is moderately or severely asphyxiated (i.e. short of oxygen due to animate bug), and the correct action that you should take. This study session is unusual in that much of it is taught through diagrams.
Learning Outcomes for Study Session 7
When you have studied this session you should be able to:
7.1 Define and use correctly all of the key words printed in bold. (SAQ vii.2)
vii.two Summarise the about of import signs of neonatal asphyxia that mean you should begin neonatal resuscitation. (SAQ seven.1)
7.3 Explain how newborns can be helped to breathe by applying standard resuscitation techniques. (SAQs 7.ane and 7.2)
7.4 Identify the equipment you will need to requite newborn resuscitation and how it should exist used correctly. (SAQ seven.iii)
vii.v Describe the things you should not do when assessing a newborn for possible animate difficulties. (SAQ 7.4)
7.six Summarise the main health risks to newborns and the activities that grade the basis of essential newborn care. (SAQ 7.5)
seven.1 Newborn respiration and resuscitation
We begin by briefly summarizing what usually happens when a newborn makes the transition from life in its mother's uterus, to life in the outside world, where it must breathe for itself.
7.i.1 Breathing in a healthy newborn
Normally, a salubrious infant starts to breath spontaneously immediately after delivery (Effigy 7.1). If the breathing started spontaneously and is sustained past the baby without assistance, it indicates that:
- The fetus was not asphyxiated while in the uterus
- The respiratory system is operation well
- The cardiovascular system (heart and blood vessels) is functioning well
- There is coordination by the brain of the movements required for sustained rhythmical breathing (encephalon is functioning well).
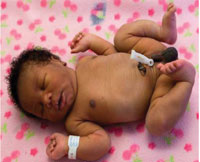
Figure 7.1 A full-term normal newborn who is breathing well has pinkish pare colour and semi-flexed arms and legs; he has made a good transition from the female parent'due south uterus to the outside globe. (Photograph: Dr Mulualem Gessese)
-
How practise you cheque fetal wellbeing during labour and delivery?
-
A salubrious fetus has a middle rate between 120–160 beats/minute. When the fetal membranes rupture, the amniotic fluid that leaks from the female parent'southward vagina is articulate, not heavily claret-stained or coloured light-green-black by meconium — the baby'south first stool.
If you checked the fetal heart rate at regular intervals all through the mother's labour, and recorded the effect on the partograph (as you learned in Study Session 4), you should have referred any mother whose unborn baby showed signs of fetal distress. Therefore, it should be relatively uncommon for y'all to deliver an asphyxiated baby. However, complications in childbirth can develop unpredictably, or you may be called to a adult female who is already far avant-garde in the 2d stage of labour when yous reach her. Therefore, you need to know how to provide neonatal resuscitation in case y'all deliver an asphyxiated baby.
7.i.two Newborn asphyxia
As yous learned in Written report Session four of this Module, asphyxia (shortage of oxygen) in the uterus is due to an inadequate supply of oxygen from the mother'due south blood or a problem in the placenta. This may result in:
- Asphyxia at nascency (mild, moderate or severe)
- Learning difficulties or cerebral impairment, which become apparent during childhood evolution; they are due to encephalon cells being destroyed by lack of oxygen during labour and commitment.
- Death of the newborn.
Gas exchange is when oxygen from the inhaled air is captivated into the blood every bit it passes through the lungs, and waste product carbon dioxide is released from the blood into the air that is breathed out
However, neonatal asphyxia is mainly due to failure of the newborn to breathe after birth, or its heart fails to pump enough blood to the lungs for gas exchange, or information technology has low haemoglobin levels (anaemia) so information technology cannot evangelize enough oxygen around the body. The baby who cannot exhale cannot establish independent life outside the mother. Therefore, the purpose of neonatal resuscitation is to assistance the newborn to establish spontaneous breathing and facilitate oxygen delivery to its organs and tissues – particularly the brain, which is very speedily damaged by oxygen shortage. You may also need to resuscitate any babe that is severely anaemic due to blood loss during labour and delivery, or that continues to exist cyanotic despite established breathing. Cyanosis is a blue discolouration of the lips and skin, which occurs when in that location is bereft oxygen in the blood (Effigy vii.2).
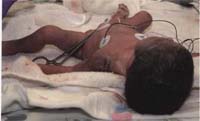
Figure 7.2 A preterm newborn with bug: she looks cyanotic (bluish), her limbs are floppy because her muscle tone is not strong, and she has breathing problems. (Photo: Dr Mulualem Gessese)
To avoid the immediate and long-term complications of asphyxia, in addition to the labour and delivery care that you lot provide to the mother, and the routine newborn care of the baby (e.g. cut the cord, keeping the babe warm), you also accept to provide life-saving interventions for any newborn who cannot breathe properly.
seven.2 Types of neonatal resuscitation
There are three techniques that yous will learn almost in this study session and in your practical skills grooming. They are:
- Ventilation: using a manus-operated pump called an ambu-bag (Figure 7.three), which pumps air into the baby's lungs through a mask fitted over its nose and mouth. (You may hear wellness professionals referring to ventilation equally 'ambu-bagging'.)
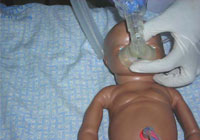
Figure 7.3 Resuscitation technique practiced with a ventilator (ambu-bag) on a preparation doll. (Photo: Dr Yifrew Berhan)
- Suctioning: using a device called a bulb syringe to extract mucus and fluid from the baby's nose and mouth.
- Centre massage: pressing on the babe's chest in a rhythmic way to stimulate the heartbeat (Effigy vii.4).
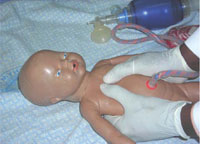
Figure vii.4 Cardiac massage technique skilful on a training doll. Yous tin see a ventilator at the top right of the flick. (Photo: Dr Yifrew Berhan)
seven.2.i Basic equipment needed for newborn resuscitation
- Two clean linen/cotton cloths: 1 to dry the newborn and one to wrap him or her afterwards
- Plastic bulb syringe to remove secretions from the rima oris and nose, specially when meconium is nowadays
- Ambu-pocketbook and mask to give oxygen directly into the baby'due south lungs
- A person trained in neonatal resuscitation (like you)
- Rut source (lamp) to provide warmth, if possible.
7.2.ii Before y'all showtime resuscitation
B efore you apply whatever course of resuscitation, make sure that:
- The baby is alive: If the newborn doesn't announced to be alive, Starting time mind to its breast with a stethoscope. If there is no heartbeat, the baby is already dead (run across Table 7.one below).
- You graded the extent of asphyxia: If you can hear a heartbeat, but you judge it to be less than 60 beats/minute, employ heart massage first, so ventilate alternately on and off, till the heartbeat is to a higher place sixty beats/minute (see Table 7.i below).
- The baby is non deeply meconium stained: If the baby's skin is stained with meconium, or the oral and nasal cavities are filled with meconium-stained fluid (Figure 7.5), y'all should not resuscitate before suctioning the oral, nasal and pharyngeal areas. Ventilation will aggravate the baby'south breathing problem because it will force the meconium-stained fluid deep into the baby'due south lungs, where it will block the gas exchange.

Figure seven.five A infant who is non breathing (no signs of chest or nose motion) and with meconium stained all over its body. (Photo: Dr Mulualem Gessese)
7.3 Assessing the degree of asphyxia
Moderate to severely asphyxiated babies usually require intensive resuscitation, then the next thing you lot have to learn is how to grade asphyxia in a newborn. Within no more than v seconds afterwards the nascence, y'all should make a very rapid assessment to observe out whether the baby is alive or dead, and (if it is alive) to assess whether it has any degree of asphyxia. A severely asphyxiated baby may non breathe at all, there may be no movement of its limbs (artillery and legs), and the skin colour may be deeply blueish or deeply white. A baby who is not animate at all after nativity, or who is only gasping for breath, or who is animate less than 30 breaths per infinitesimal needs help immediately. If a baby does not exhale soon after birth, it may become brain damage or dice. Well-nigh babies who are not breathing can exist saved if resuscitated correctly and apace.
From Table 7.1, yous tin larn how to assess a newborn's degree of asphyxia. Also look again at the iii photos of newborns with different level of asphyxia (Figures vii.1, seven.2 and vii.5).
Gasping is when the newborn tin can take only a few breaths with difficulty and with wide gaps in between; it is commonly a sign that the baby is close to decease.
Table 7.1 Assessing the degree of asphyxia.
| Signs | No asphyxia | Mild asphyxia | Moderate asphyxia | Severe asphyxia |
|---|---|---|---|---|
| Heart charge per unit | Above 100 beats/infinitesimal | Above 100 beats/minute | Higher up threescore beats/minute | Beneath lx beats/infinitesimal |
| Skin colour | Pink | Balmy blueish | Moderately blueish | Securely blue |
| Breathing design | Crying | Crying | Breathing but not potent | Non animate, or gasping type |
| Limb movement | Moving well | Weakly moving | Floppy | Floppy |
| Meconium-stained | No | No | Perchance | Commonly |
| Resuscitation | No need | Fast response | Good response | Takes a long fourth dimension to respond |
![]() Assessment of the degree of asphyxia should not take you more than than 5 seconds. Do it fast but don't panic.
Assessment of the degree of asphyxia should not take you more than than 5 seconds. Do it fast but don't panic.
Since neonatal resuscitation is an activeness that yous need to perform chop-chop (within 1 minute after delivery), information technology is ameliorate to judge than to count the heart rate, and to observe the pattern of breathing rather than to count the respiratory rate. Table seven.2 gives yous a simplified description of the signs that signal what is normal and aberrant immediately after birth.
Table vii.two Normal and abnormal physical findings in the newborn immediately after nascency.
| Signs | Normal findings | Abnormal findings |
|---|---|---|
| Colour | Should be pinkish | Blue or cyanosed (shortage of oxygen) White, pallor (anaemia) Yellowish (jaundice) |
| Animate | forty–60 breaths/minute | No breathing Breathing rate less than 30/minute Gasping (very few breaths with difficulty breathing) |
| Heart rate | 120–160 beats/infinitesimal | No heartbeat at all Heartbeat less than 100/infinitesimal |
| Muscle tone | Full term newborn has semi-flexed arms and legs (Effigy 7.1) | Poor flexion of the limbs; arms and legs floppy (Effigy 7.2), indicates moderate to severe asphyxia affecting the brain |
| Reflexes | Infant responds to a finger put into the roof of its oral fissure | No response to touching the roof of the baby's mouth |
'Less than' can exist replaced by the < symbol, as in <30/min. 'More than' tin can exist replaced by the > symbol, equally in >30/min.
vii.4 Neonatal resuscitation procedures
Before you become to attend whatever delivery, you should make certain that y'all have prepared the equipment necessary to apply neonatal resuscitation and give immediate intendance to the newborn if required. In this section we move on to the actions that y'all should accept one time you accept assessed the caste of asphyxia.
7.4.one The first v seconds
Table 7.3 summarises what you should do in the first v seconds after the baby is born if the signs of asphyxia are present. After you have seen this overview, we will expect at the specific actions in detail.
Tabular array 7.3 Actions in response to signs of neonatal asphyxia.
| What is the newborn doing? | Assessment | Action |
|---|---|---|
| Crying and moving limbs | Probably a healthy infant | Resuscitation not needed |
| Weak breathing, not moving limbs, moderate cyanosis | Probably moderately asphyxiated | Help breathing past on and off ventilation (equally described in Section 7.four.8) |
| Non crying, animate or gasping; not moving limbs/floppy; may exist cyanosed or meconium stained | Probably severely asphyxiated | Estimate heart charge per unit Call an assistant (family member or other) Suction the oral, nasal and pharyngeal area in less than 5 seconds using a bulb syringe On and off ventilation |
| As in a higher place | Heart rate to a higher place 60 beats/minute | |
| As above | Heart charge per unit below 60 beats/minute | Equally higher up, simply with the addition of cardiac massage (see Figure 7.four) |
7.4.ii Checking the newborn'southward centre rate
The apical heart beat (or AHB) is just another name for the heartbeat heard through a stethoscope over the area of the heart on the left side of the breast, every bit shown in Figure seven.half-dozen. It is called 'apical' because the heartbeat is heard straight from the surface of the heart.
-
What is the proper name given to the number of heartbeats per minute measured away from the the heart?
-
It is chosen the pulse charge per unit.
The newborn's heartbeats can also be counted past feeling the pulse at the base of the umbilical cord, as shown in Figure 7.six.
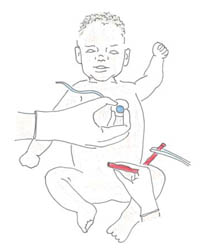
Figure 7.7 Checking and counting the upmost heartbeat (AHB) and feeling for the pulse at the base of the umbilical cord.
7.4.three The initial deportment
The listing below sets out the actions you should accept for all newborns in the sequence shown, irrespective of the degree of asphyxia:
- Fast drying as shown in Figure seven.8
- Keeping the baby warm.
- Clearing the oral cavity and olfactory organ as shown in Effigy vii.nine
- Apply gentle tactile stimulation to initiate or heighten breathing equally shown in Figure 7.10
- Simultaneously assessing the caste of asphyxia every bit shown earlier in Tables 7.ane to 7.3
- Positioning the babe for resuscitation if there are signs of asphyxia, as shown in Figure seven.11
At present study each of these figures in turn. Wait at them advisedly and brand certain that you read the captions and other notes associated with them.
7.4.iv Dry the babe chop-chop and keep it warm
Lay the baby on a warm surface away from drafts. Use a estrus lamp or other overhead warmer, if available. Then dry out the baby every bit shown in Figure 7.8.
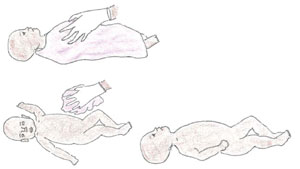
Effigy vii.8 How to dry out the baby: (top) lay the babe on its back and dry out it thoroughly; (bottom left) remove the wet cloth; (bottom right) tilt the baby's chin to reposition the babe'southward caput and continue its airway open.
Place the baby in pare-to-peel contact with the female parent, covered by a warm coating. Place a warm cap or shawl to embrace the baby'due south head.
vii.four.v Clearing the mouth and nose
If a bulb syringe is bachelor:
![]() Suction the oral fissure offset, then the baby's nose ('m' before 'n') — see Figure vii.9.
Suction the oral fissure offset, then the baby's nose ('m' before 'n') — see Figure vii.9.
No deep suctioning with a bulb syringe! Information technology can cause slowing of the eye rate (bradycardia).
If no seedling syringe:
Clear secretions from the rima oris and nose with a clean, dry fabric.
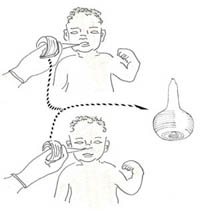
Figure vii.9 Suctioning the newborn with a seedling syringe to articulate fungus from its upper airway: (pinnacle) suction the rima oris beginning; (bottom) and then suction the babe'due south olfactory organ ('grand' before 'n').
7.4.6 Apply gentle tactile stimulation to initiate or heighten animate
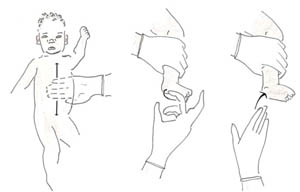
Figure 7.10 How to requite gentle tactile stimulation: (left) rub the baby'southward belly up and down; (centre and right) flick the underside of the babe'southward foot with your fingers.
![]() DO NOT stimulate by:
DO NOT stimulate by:
These types of stimulation are dangerous and tin can damage the newborn.
- Slapping the back
- Squeezing the rib cage
- Forcing the baby'southward thighs into its abdomen
- Dilating the anal sphincter (the ring of muscle that closes the anus)
- Hot or cold compresses or baths
- Shaking the umbilical string.
7.4.seven If you diagnose asphyxia, get-go resuscitation!
Position the newborn on his or her back with the neck slightly extended as shown in the top picture in Figure vii.xi. Open the airway past immigration the oral cavity and nose with suction using the bulb syringe as you saw previously in Effigy 7.9.
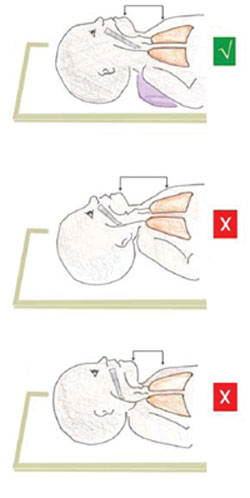
Effigy vii.11 How to position the newborn's head to keep its airway open: (top) correct, the baby's chin is tilted the right corporeality; (middle) the babe's head is tilted also far back, placing pressure level on the windpipe in its cervix; (bottom) the infant's head is non tilted plenty — its chin is besides close to its chest and the airway is compressed.
- Position yourself at the head of the baby (meet Figure 7.12).
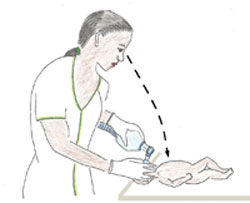
Effigy seven.12 The right position for newborn resuscitation using an ambu-bag.
If the api cal heart vanquish is > (more than) threescore beats/minute:
- Ventilate with the appropriate size of mask and a cocky-inflating ambu-purse. The mask should exist fitted every bit shown in Figure seven.13. Make a firm seal betwixt the mask and the infant's face up, so air cannot escape from nether the edges of the mask. Only don't force the mask downwards onto the baby's face, because this could button its mentum downwards towards its chest (bottom diagram in Effigy seven.11) and compress its airway.
If the apical heart beat out is < (less than) 60 beats/minute:
- Apply middle massage (expect back at Figure vii.4) and ventilate alternately (on and off ventilation) with the ambu-bag.
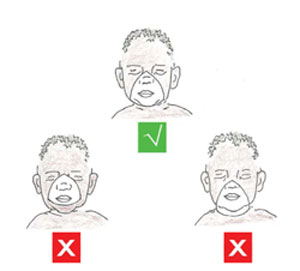
Figure 7.13 Right and incorrect size of mask: (top) correct: Covers mouth, nose, and chin; (bottom left) incorrect: besides large — covers eyes and extends over chin; (bottom right) wrong: too small-scale — does non cover nose and oral cavity.
seven.4.8 Ventilate at forty breaths per minute
Count out loud: 'Breathe — ii — three' as yous ventilate the baby (run into Effigy 7.xiv). Clasp the purse as you say 'Breathe' and release the pressure level on the handbag every bit you say 'two — three'. This helps y'all to ventilate with an fifty-fifty rhythm, at a rate that the newborn's lungs are naturally adjusted to.
The amount of air you are moving into and out of the lungs is the equivalent of near twoscore breaths per minute. Utilize enough pressure to create a noticeable, gentle ascension and fall in the babe's chest. The starting time few breaths may require higher pressures, but if the babe appears to exist taking a very deep breath, you are using too much pressure level.
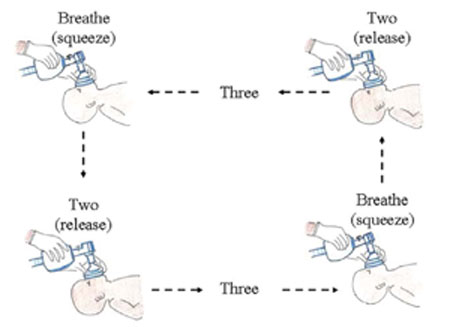
Figure 7.14 Timing the rate of ventilation equally y'all say 'Breathe — two — iii'.
7.4.nine Evaluate the baby during ventilation
The all-time sign of skilful ventilation and comeback in the baby's condition is an increase in eye rate to more than than 100 beats/minute.
-
What other change would yous expect to come across in the baby while yous are ventilating it, if the resuscitation is going well?
-
You would expect to see the baby's skin color change from blue or very stake, to a healthier pinkish color. You may also run into the baby begin to move a niggling fleck, beginning to flex its limbs and await less floppy.
When yous terminate ventilating for a moment, is the baby capable of spontaneous animate or crying? These are good signs. Many babies recover very quickly after a short flow of ventilation, merely continue closely monitoring the baby until you are sure it is breathing well on its own.
If the baby remains weak or is having irregular breathing afterward 30 minutes of resuscitation, refer the mother and infant urgently to a health centre or infirmary where they accept facilities to help babies who are having difficulty breathing. Go with them and keep ventilating the baby all the fashion. Make sure it is kept warm at all times. Newborns easily lose heat and this could be fatal in a babe that can't exhale adequately on its own.
Figure seven.15 summarises the steps in newborn resuscitation which yous accept learned in Section 7.4.
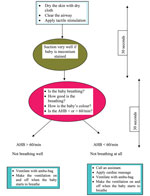
Figure 7.15 A summary of the steps in newborn resuscitation in the form of a flow chart.
7.5 Firsthand essential newborn intendance
We end this written report session with a reminder about essential newborn care, which you should conduct with all babies, regardless of whether they take any signs of asphyxiation. When the baby's umbilical cord is cut, there are many physiological changes inside the baby's trunk to allow information technology to make the necessary accommodation to life outside its mother. Information technology is generally tougher to survive in the outside globe than in the relative prophylactic of the uterus, and so we need to provide basic care to the newborn to help it resist some potential health risks listed in Box vii.one.
Box 7.1 Wellness risks to newborns
Newborns demand additional care to prevent:
- Spontaneous bleeding, unremarkably from the gastrointestinal tract, due to Vitamin K deficiency
- Bleeding due to birth trauma (usually manifested belatedly afterwards delivery with swelling over scalp that requires firsthand referral)
- Heart infections due to Chlamydia trachomatis and Neisseria gonorrhea (leaner which are mutual causes of sexually transmitted infections; the babe can acquire these infections as it passes through the birth culvert)
- Some vaccine preventable diseases such as poliomyelitis and tuberculosis
- Hypothermia (becoming likewise cold)
- Hypoglycaemia (low blood glucose level)
- Mother-to-child transmission of HIV, if the mother is HIV-positive.
Vaccine preventable diseases are discussed in detail in the Catching Diseases Module, Report Sessions 3 and 4.
Prevention of mother-to-child transmission (PMTCT) of HIV is covered in the Antenatal Care Module, Study Session 17; the drugs and procedures for PMTCT are given in the Infectious disease Module, Study Session 27.
With the health risks in Box seven.i in mind, make certain that you give all newborn babies the following essential care:
- Tie the umbilical cord two finger-widths from the babe's belly and place a second tie two finger-widths away from the start one. Cut the string betwixt the first and 2d ties. Bank check that the umbilical string stump is not haemorrhage and is non cutting likewise curt
- Employ tetracycline eye ointment in one case only, to prevent eye infections.
- Inject vitamin K (1 mg, intramuscularly) into the front of the infant's mid-thigh to foreclose spontaneous bleeding.
- Requite the first dose of oral polio vaccine and BCG vaccine (confronting tuberculosis) according to the guidelines in the Ethiopian Expanded Programme of Immunization (EPI).
- The trunk temperature of the newborn must remain higher up 36oC. Place the infant on the mother's abdomen in peel-to-pare contact with her, where it can breastfeed. Cover them both with a coating and put a warm hat or shawl over the baby's head.
- Ensure that the baby is suckling well and the mother's chest is producing adequate milk. If breastmilk is not preferred, make sure that adequate replacement feeding is ready. Initiate early and exclusive breastfeeding unless there are skillful reasons to avoid it, e.g. in an HIV-positive mother.
- The babe should become preventive treatment to protect it from HIV if its mother is HIV-positive.
The vaccination schedule for all the vaccines in the EPI are described in total in the Immunization Module.
You will learn all nigh breastfeeding in the Postnatal Care Module. Breastfeeding and HIV are covered in the Infectious disease Module, Study Session 27.
Summary of Study Session 7
In Study Session 7, you have learned that:
- The well-nigh of import signs of asphyxiation in newborns at delivery are: difficulty breathing, gasping or no breathing; abnormal middle crush; poor muscle tone (floppy limbs); lack of movement; bluish pare colour (cyanosis), and existence stained with meconium.
- Assessment of the degree of asphyxia should exist done in the get-go 5 seconds subsequently the birth, at the aforementioned time as commencing basic newborn care (e.one thousand. drying the baby, keeping it warm, tying and cutting the string, etc).
- Swift action is necessary to begin resuscitating a baby who is not breathing well, after you have suctioned its rima oris and so its nose.
- Cheque that the infant is alive (mind for an apical heartbeat); that the heart rate is to a higher place 60 beats/infinitesimal (begin middle massage before resuscitation if the heart charge per unit is less than 60 beats/minute); and that the baby is not stained with meconium, which must be suctioned out before resuscitation can begin.
- Position the baby with its cervix extended to open the airways; place a correctly fitting ventilation mask over the baby'south mouth and olfactory organ, and brainstorm ventilating at a rate of well-nigh xl breaths per infinitesimal.
- Watch for signs of improvement: e.g. pinkish colour, motility, power to breathe unaided, etc. Refer urgently if this has non been achieved after 30 minutes of ventilation.
- Recall to behave all the activities of essential newborn intendance, including cord care, giving a vitamin Thou injection and tetracycline eye ointment, establishing early and exclusive breastfeeding, and ensuring that anti-HIV medication is given to foreclose mother-to-child-transmission.
Cocky-Assessment Questions (SAQs) for Study Session seven
Now that you accept completed this study session, you can assess how well you have accomplished its Learning Outcomes past answering the following questions. Write your answers in your Study Diary and discuss them with your Tutor at the side by side Study Back up Meeting. You can check your answers with the Notes on the Self-Assessment Questions at the cease of this Module.
First read Case Written report 7.1 and so answer the questions that follow it.
Case Study 7.1 Atsede'south infant can't exhale
A 25 year-old adult female called Atsede was brought to your Wellness Postal service after being in labour for 38 hours at home. Presently later she reached y'all, she gave nascency to a full term baby boy. You assessed the baby and found he was not making whatsoever breathing effort, he had no movement of his limbs and his whole torso was covered with meconium-stained amniotic fluid. When you stale him and applied tactile stimulation, the baby all the same didn't testify any effort to exhale.
SAQ 7.1 (tests Learning Outcomes seven.2 and 7.3)
- a.Is this baby asphyxiated? If yes, what is the caste of asphyxia?
- b.What are your immediate adjacent steps? Then what practise you do?
- c.Could the nascence complication in this newborn have been prevented, and if so, how?
Answer
- a.Atsede'south baby is severely asphyxiated. The danger signs are that he was non making any breathing try, or moving his limbs, he was covered with meconium and tactile stimulation had no consequence.
- b.Your next step is to dry out him quickly, wrap him warmly, and remove meconium from his rima oris and olfactory organ with the bulb syringe and a make clean textile. Listen for an apical heartbeat and if it is below threescore beats/minute, begin heart massage, alternate with ventilating the baby at almost 40 breaths per minute.
- c.The nascence complication in this newborn could have been prevented by Atsede receiving skilled birth attendance much earlier in her labour from someone who could monitor the signs of fetal distress and refer her for emergency care; 38 hours is as well long to expect.
SAQ 7.2 (tests Learning Outcomes 7.4
List the basic equipment you will need in society to resuscitate a newborn with breathing difficulties.
Answer
The basic equipment you will demand in order to resuscitate a newborn with breathing difficulties are:
- Two make clean linen/cotton cloths: one to dry the newborn and one to wrap him or her later on
- Plastic bulb syringe to remove secretions from the mouth and nose, peculiarly when meconium is present
- Ambu-handbag and mask to give oxygen directly into the infant'southward lungs
- A person trained in neonatal resuscitation (like you)
- Rut source (lamp) to provide warmth, if possible.
SAQ seven.3 (tests Learning Outcomes 7.1, seven.two, 7.four, seven.five and seven.6)
Which of the post-obit statements is faux? In each case say what is incorrect.
A If a newborn cries soon later birth, it is a sign of asphyxia occurring before delivery.
B Cyanosis means being covered with meconium all over the trunk.
C The upmost heartbeat can exist detected by listening to the baby's chest with a stethoscope.
D Gas commutation in the lungs happens when carbon dioxide is breathed in and oxygen is breathed out.
East Giving the newborn a Vitamin K injection is to prevent centre infections.
F The recommended ventilation charge per unit for newborns is forty breaths/minute.
Answer
A is false. If a newborn cries soon after birth, it is a sign of asphyxia occurring before delivery.
B is false. Cyanosis means having a bluish colour to the pare because of oxygen shortage (asphyxia).
C is true. The upmost heartbeat can exist detected by listening to the baby'due south chest with a stethoscope.
D is fake. Gas commutation in the lungs happens when carbon dioxide is breathed out and oxygen is breathed in.
E is faux. Giving the newborn a vitamin K injection is to prevent spontaneous bleeding; tetracycline ointment is given to foreclose eye infections.
F is true. The recommended ventilation rate for newborns is 40 breaths/minute.
SAQ vii.iv (tests Learning Consequence 7.iv)
Which of the following ways of stimulating the newborn are recommended, and which are dangerous and not allowed?
- Slapping the back
- Rubbing the abdomen gently up and down
- Squeezing the rib cage
- Forcing thighs into the abdomen
- Flicking the underside of the babe's human foot with your fingers
- Dilating the anal sphincter
- Hot or cold compresses or baths
- Shaking the umbilical string.
Answer
Only ii of the means in the list are recommended for gentle tactile stimulation of the babe:
- Rubbing the abdomen gently up and down
- Flicking the underside of the infant'due south foot with your fingers.
All the other ways listed are dangerous and should non happen.
SAQ 7.five
Table seven.1 summarises some common health risks to newborns and the firsthand essential intendance to prevent those complications. Some of the boxes have been left blank for you to consummate.
Table 7.1 for use with SAQ 7.5
| Newborn health risk | Essential newborn care |
|---|---|
| Eye infection | |
| Spontaneous bleeding | |
| Hypothermia | |
| Hypoglycaemia |
Answer
The completed Table 7.1 is below.
Table 7.ane Completed
| Newborn health risk | Essential newborn care |
|---|---|
| Eye infection | Use tetracycline eye ointment |
| Spontaneous bleeding | Inject 1 mg vitamin K intramuscularly |
| Skin-to-skin contact with mother, blankets and cap | Hypothermia |
| Early on breastfeeding or adequate replacement feeding | Hypoglycaemia |
mcauleyanardeakin.blogspot.com
Source: https://www.open.edu/openlearncreate/mod/oucontent/view.php?id=275&printable=1
Postar um comentário for "Why Do You Suction a Baby's Mouth First"